Leaking urine is not normal. Being unable to urinate or still feeling the urge to pee even though you had just gone to the toilet is also not normal.
Here’s some deeper insight to what urine incontinence is.
Types of Urine Incontinence
1) Stress Incontinence: This is when you leak urine as you cough, sneeze, laugh, play sports/heavy lifting, or do certain movements that strains your body. It happens because your urethral sphincter and pelvic floor muscles are weak and can not hold the urethra closed under pressure, so as you cough or sneeze, or do anything that increases your intra-abdominal pressure, this adds pressure upon your urethral sphincter, and hence it leaks urine.
Stress incontinence can also be due to a dysfunctional urethral sphincter, caused maybe from an accident or long-term stress (like holding your urine for long hours for a long-term period) or other factors.
2) Urge Incontinence: This is when you have sudden involuntary loss of urine. The main cause is due to overactivity of muscles in your bladder, which causes voiding of urine. Sometimes the urine just expels without urge or warning, sometimes it can be triggered by the sound of running water, the sight of a toilet sign, or even when you are on the way to the toilet.
3) Mixed incontinence: This is a mixture of stress and urge incontinence.
4) Neurogenic Incontinence: This has symptoms similar to the other types of incontinence, but its cause is due to nerve damage, either in the brain, spinal cord or a nerve pathway.
5) Overflow Incontinence: This is when there is urine leakage due to the bladder being too full because of an obstruction in the urethra. You may leak in small amounts periodically or continuously, and even after emptying your bladder, you may still feel like it is full. Sometimes the urge to pee keeps coming but you are unable to urinate.

How Physiotherapy Helps
For urinary incontinence, the kind of physiotherapy rehab required depends on the type of incontinence, but essentially there are several main components, areas, that are involved and would be targeted.
1- High intra-abdominal pressure. Here, we will want to target the regulation of the intra-abdominal pressure, looking at breathing techniques. It’s important to ensure you are breathing deep and strong, using your diaphragm and not your accessory breathing muscles as your main breathing muscle. As your diaphragm contracts and relaxes, the intra-abdominal pressure changes accordingly, and your pelvic floor muscles, too, play a part in this regulation.
Sometimes the pelvic floor muscles are tight, decreasing space and leeway for movement, hence increasing intra-abdominal pressure. Thus, another aspect to look aside from breathing technique is the tightness of pelvic floor muscles. Learning reversed kegel exercises is key in relaxing the pelvic floor muscles. Reversed kegels along with deep breathing with your diaphragm is very important to help regulate your intra-abdominal pressure, but we will need to be a little careful here, as reversed kegels may not be advisable at the start of recovering from stress incontinence, as it can cause a little too much stretch to the already weak pelvic floor muscles. Best visit to check with us at Relive Physio, to advise you accordingly.

2- Weak and/or tight pelvic floor muscles: For pelvic muscle weakness, kegel exercises are important to strengthen your pelvic floor muscles, to improve the strength of the urethral sphincter. If pelvic floor muscles are tight, manual release and stretches are advisable. Reversed kegels are important to practice when having tight pelvic floor muscles.
Often, pelvic floor muscles can be weak and tight, this requires a good balance of learning to apply kegels and reversed kegels, but how and when to apply, this should be advised by the pelvic health therapist as he/she journeys along with you in rehab.

3- Surrounding hip/thigh muscles: It’s also important to look at the surrounding muscles, in the glutes or thighs, to see whether there is a need to stretch tight muscles and/or strengthen weak muscles. A few important muscles to look at are the piriformis, gluteus maximus, hip adductors, hamstrings. These muscles may be tight and/or compensating movement meant to be executed by the pelvic floor muscles.
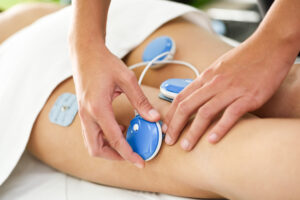
4- Neuro sensitivity/de-sensitise: Electrical modalities, such as TENS, are used here to stimulate nerves or desensitise over-stimulated nerves, such as relaxing an overactive bladder, in urge incontinence.

What's Next?
If you are experiencing difficulty in urinating or struggling with urinal urges, do not wait longer to do something about it!
Feel free to drop by for a session with our woman’s health specialist. Or you can contact us via Whatsapp, and let us know how we can help you!
Bonus Content!
1) Can Urinary Tract Infection (UTI) lead to urinary incontinence?
Answer: Yes, it can. It can be vice versa as well.
2) Is full recovery from Urine Incontinence possible? How long does recovery take?
Answer: Generally, urinary incontinence recovery depends on several factors – the cause, the complications, the condition and health of the body. It can be possible to fully recover, and if so, the next question for that would be, how long would that take? It can take from a few weeks to several months. Sometimes, it’s not possible to fully recover but to be better and to feel more comfortable, or at least to maintain the state of the condition, so that it does not deteriorate.




